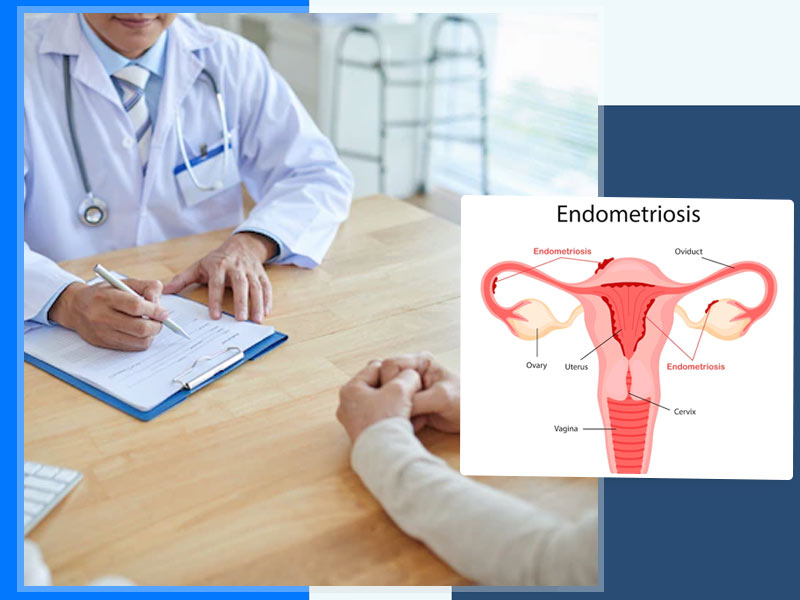
Endometriosis is a condition where tissue similar to the lining of uterus is found outside the uterus at ectopic locations and causes painful periods, infertility, chronic pelvic pain, fatigue, bowel symptoms, urinary symptoms, painful sex and many other symptoms. It affects 1 in 10 women and globally 200 million women are suffering with endometriosis. Currently there is no cure for endometriosis but treatment is tailored to one’s needs and requirements. As per Dr. Vimee Bindra - Fertility Enhancing Surgery Specialist, Endometriosis Excision Surgery Specialist & Co-Founder-ENDOCRUSADERS, doctors consider several factors before recommending certain type of treatment for endometriosis such as age, severity of symptoms, severity of disease, organ involvement such as bladder and bowel involvement and whether one desires to have children.
Table of Content:-
Medical treatment for endometriosis
Usually medical therapy is not a cure for endometriosis but while you use them your symptoms may reduce but once stopped they may come back. Endometriosis is a progressive disease and if on medical therapy one has to strictly monitor the interval growth of endometriotic lesions as progressive lesions may cause permanent organ damage in some cases. These are suitable for endometriosis pain management.

Pain medications
If symptoms are mild pain medications may work but for endometriosis chronic pain, over the counter analgesics don’t work and it’s an indication that the cause of your severe pain could be endometriosis. The most common pain relievers are NSAIDS.
Hormone therapy
Hormone therapy is widely used for endometriosis treatment but it’s not an effective treatment and it may reduce your symptoms temporarily. Hormonal therapy works by stopping the ovaries from producing hormones and prevent ovulation. This produces anovulation and pseudo-menopause and patients may get relief from pain but disease does not disappear.
Also Read: Endometriosis And Stomach Pain During Period
Following hormones are widely prescribed:
GnRH analogues – it produces a state of menopause in the body and it is believed that it stops the growth of endometriosis but as soon as it is stopped the lesions start growing again. This has short and long term side effects headache, nausea, hot flushes, difficulty sleeping, absence of periods, anxiety, depression, joint pain, memory loss and bone loss.

Oral contraceptives or birth control pills
These pills contain two hormones estrogen and progesterone. These pills inhibit ovulation, make cycles regular, lighter and patient report relative relief from pain when on oral contraceptive pills. Pill may not be suitable for everyone and like any other hormonal treatment pain relief lasts only when taking the pills and symptoms may return when discontinued. Occasionally some women may have no pain even after stopping endometriosis treatment. These hormones can have mild side effects such as bloating, intermenstrual bleeding and nausea.
Progesterone based medications
These can be prescribed in the form of a pill, injection or intra-uterine device (Mirena).
- Pill is prescribed as a daily progesterone which reduces menstrual flow. As soon as pill is stopped symptoms may return.
- Mirena or intra-uterine device may be effective in reducing symptoms such as pain and excessive bleeding associated with endometriosis. It’s a contraceptive as well so not suitable for patients planning for pregnancy. It may also reduce the number of periods one gets or may not get period at all. (one third of women no longer get their period after a year of use)
Progesterone injections are prescribed every 3 months. Some women may experience irregular bleeding with these injections and may cause absence of periods in 50 % of women after using it for a year. It may cause depression, weight gain, bone loss on long term use, irregular vaginal bleeding.
Also Read: What Is The Connection Between Endometriosis And Infertility?

Endometriosis treatment surgery
Laparoscopy is considered gold standard for diagnosing and treating endometriosis. Evidence shows excision surgery for endometriosis can provide significant relief from pain, enhances spontaneous pregnancy rates and also enhances assisted reproduction rates. It is important that surgery is done by an endometriosis expert who leads a multi-disciplinary team and all your endometriosis at different locations is addressed at the same time. The surgical plan should be discussed in detail before surgery and how best it can enhance your fertility and reduce pain at the same time depending on the patient.
Laparoscopy or robotic surgery
This is a minimally invasive way of doing surgery where all endometriotic lesions or nodules are excised either by laparoscopy or robotic surgery. The robotic and laparoscopy are the tools operated by an expert. So your surgeon should be well versed with the tool which they are using and provide you the best outcome.
Also Read: Why You’re Not Getting Pregnant? Here Are 8 Reasons for Female Infertility

In this abdomen is inflated with a harmless gas carbon dioxide and small instruments or robotic arms are introduced through small incisions/ cuts on the abdomen and endometriosis surgeon removes the lesions through a process called excision. Many gynaecologists use a technique where lesions are burnt and its called ablation. This treatment is NOT effective as endometriotic lesions are deeper than they appear so surface is ablated but deeper disease is left behind.
The goal of laparoscopic surgery is to be radical nerve sparing surgery while maintaining the organ function and enhance fertility for patients who wish to become pregnant and provide patients with a good quality of life.
Treatment options for infertility due to endometriosis
In most cases after excision surgery, spontaneous fertility rates are improved. If pregnancy does not occur, in vitro fertilization may be the best option to enhance the chances. Fertility potential of a patient with endometriosis depends on a lot of factors such as ovarian reserve and antral follicle count. For patients who have low ovarian reserve may be offered oocyte or embryo freezing before surgery and embryo transfer can done after surgical excision. Treatment needs to be tailored to one needs AS ONE SIZE DOES NOT FIT ALL.
Image credits- freepik
Also watch this video
How we keep this article up to date:
We work with experts and keep a close eye on the latest in health and wellness. Whenever there is a new research or helpful information, we update our articles with accurate and useful advice.
Current Version