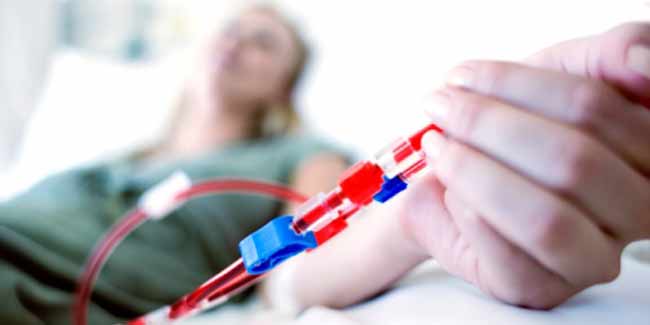
Dialysis can save lives of patients suffering from end stage renal disease (ESRD). However, this life-saving treatment may pose side-effects in case of peritoneal dialysis (PD) and haemodialysis.
Factors like the patient’s condition and whether or not they are following their dietary and fluid restrictions may influence the intensity of side-effects from mild to severe. If the patient follows healthcare team’s instructions carefully, they can successfully manage most of these side-effects.
Table of Content:-
Side-effects of peritoneal dialysis (PD)

Infection
PD is a home dialysis procedure categorised into three types – continuous ambulatory dialysis (CAPD), continuous cycler-assisted peritoneal dialysis (CCPD) and nocturnal intermittent peritoneal dialysis (NIPD). All these types need a small rubber tube called a catheter to be inserted. In order to allow the dialysis solution to move into and out of the abdominal cavity, the catheter is positioned inside and outside of the body. The exchange of dialysis solution can give rise to infection.
The patient may suffer fever, nausea, vomiting and stomach pain, as symptoms of peritonitis (inflammation of the peritoneum, typically caused by bacterial infection either via the blood or after rupture of an abdominal organ). The dialysis solution may also look cloudy. To stop the infection from spreading further, peritonitis must be treated quickly.
Performing the procedure in a clean area should mitigate the chances of an infection. Patients may be prescribed to apply antibiotics at the catheter’s exit site.
Hernia
Another potential side-effect of PD is hernia. Insertion of the catheter can weaken abdominal wall muscles that protect internal organs and keep them in place. During an exchange, the pressure from the dialysis solution in the peritoneum can push further against muscles that are already weak. Because of this pressure, a tear could develop and organs from the abdominal cavity may emerge through the opening. The only way to treat a hernia is surgery.
Bloating and weight gain
Many patients on PD complain of bloating and weight gain. Dialysis solution sitting in the peritoneum could be causing some of this weight gain or fluid bloat. The sugar in the dialysis solution absorbed by the body can also cause weight gain. A renal dietician can teach you how to balance nutritional needs and achieve comfort.
Side-effects of haemodialysis
Low blood pressure
Low blood pressure is the most common side-effect of haemodialysis. It occurs when excessive fluid is removed from blood during the procedure. The blood pressure drops, causing nausea and dizziness. You must inform your dialysis team if you experience any such symptoms. Do not take medications for high blood pressure before treatment unless your doctor has prescribed it that way.
Cramps
Patients undergoing haemodialysis may sometimes suffer muscle cramps when the fluid is taken out of the body at a fast rate or if too much fluid is removed. Your doctor may be able to help you with a solution.
Infection
Haemodialysis can also infect or inflame an access (either a fistula or a graft). The site may become infected because of the pressure cast on the access. Keep the area clean to prevent an infection.
Itchy skin
Dialysis doesn’t effectively remove phosphorus, which could be a reason (along with others) behind itchy skin. This is why patients on a renal diet are asked to leave phosphorus-rich foods. Following the recommended diet and taking a phosphorus binder can help prevent this side-effect.
Blow to sexual desire
Dialysis may also affect your sexuality by causing loss of desire, erectile dysfunction and vaginal dryness. Patients might also have to deal with anxiety, depression and change in self-image, all of which may decrease sexual drive.
Any such symptoms should be reported to the doctor so you can manage these side-effects of kidney dialysis treatment better.
Image Source: Getty
Read more articles on Understand Peritoneal Dialysis.
Read Next
Eye flu treatment by expert
How we keep this article up to date:
We work with experts and keep a close eye on the latest in health and wellness. Whenever there is a new research or helpful information, we update our articles with accurate and useful advice.
Current Version