
Coronary angioplasty is a common medical procedure done in people with coronary heart disease. It is a safe procedure and serious complications are rare. Like any other medical procedure, some complications can occur no matter how experienced and careful your doctor is or how well the procedure is done.
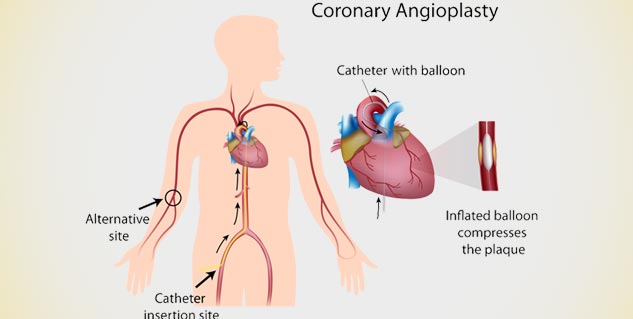
Common complications of angioplasty include:
- Pain and/or bleeding at the catheter insertion site (the place from where the catheter is threaded into the affected coronary artery).
- Damage to blood vessel from the catheters.
- Allergic reaction to the dye used for angioplasty.
- Arrhythmia (or irregular heartbeat).
- Fall of blood pressure.
- Failure of procedure and need for emergency coronary artery bypass grafting (during the procedure). This complication, however, is rare and occurs in less than 3 percent of people. It may happen if an artery closes down instead of opening up.
- Kidney damage due to dye used for angioplasty.
- Heart attack (can occur in about 3–5 percent of people).
- Stroke (occurs in less than 1 percent of people).
- It can be fatal like any procedure involving the heart. This complication occurs in less than 2 percent of people during the procedure.
Some people may have chest pain during angioplasty when the balloon is inflated and the blood supply to the heart is briefly interrupted.
Some factors, which increase the risk of complications, are:
- Age: more common in people aged 65 and older.
- Chronic kidney disease.
- Presence of shock.
- Presence of extensive heart disease and blockages in the coronary (heart) arteries.
Complications from Stents: A small mesh tube called a stent is placed in the coronary artery after the balloon is inflated in angioplasty. The stent is helpful as it supports the inner artery wall and decreases the risk of artery becoming narrow or blocked again.
- Restenosis: After angioplasty, if excessive tissue growth occurs within the treated portion of the artery, it can become narrow or blocked again. This complication is called restenosis and often occurs within 6 months. Restenosis is more common if the stent (small mesh tube) isn't used during angioplasty (30 percent have restenosis). About 15 percent of people have restenosis if a stent is used. Newer stents called drug-eluting stents (stents coated with medicine, which is slowly and continuously released into the artery) reduce the growth of scar tissue around the stent. About 10 percent of people have restenosis if a drug-eluting stent is used.
- Blood Clots: The risk of blood clot formation is higher in medicine-coated stents compared with bare metal stents. After inserting a medicine-coated stent, your doctor will recommend antiplatelet medicines such as clopidogrel and aspirin for up to a year or longer. If you take medicines as recommended by your doctor, you may be at a lower risk of blood clot formation.
Read Next
Treatment of High Blood Pressure
How we keep this article up to date:
We work with experts and keep a close eye on the latest in health and wellness. Whenever there is a new research or helpful information, we update our articles with accurate and useful advice.
Current Version
