
Many holes in the heart don't need treatment, but some do. Most holes in the heart that need treatment are repaired in infancy or early childhood. Sometimes, adults are treated for holes in the heart if problems develop.
Table of Content:-
The treatment your child receives depends on the type, location, and size of the hole. Other factors include your child's age, size, and general health.
Treating Atrial Septal Defect
Periodic checkups are done to see whether an atrial septal defect (ASD) closes on its own. About half of all ASDs close on their own over time, and about 20 percent close within the first year of life.
Your child's doctor will let you know how often your child should have checkups. For an ASD, frequent checkups aren't needed.
When treatment of an ASD is required, it involves catheter or surgical procedures to close the hole. Doctors often decide to close an ASD in children who still have medium to large holes by the time they're 2 to 5 years old.
Catheter Procedure
Until the early 1990s, surgery was the usual method for closing all ASDs. Now, thanks to medical advances, doctors can use catheter procedures to close secundum ASDs, the most common type of ASD. For this procedure, your child is given medicine so he or she will sleep through it and not feel any pain.
During the procedure, the doctor inserts a catheter (a thin, flexible tube) into a vein in the groin (upper thigh) and threads it to the heart's septum. The catheter has a tiny umbrella-like device folded up inside it.
When the catheter reaches the septum, the device is pushed out of the catheter and positioned so that it plugs the hole between the atria. The device is secured in place and the catheter is withdrawn from the body.
Within 6 months, normal tissue grows in and over the device. There is no need to replace the closure device as the child grows.
Doctors often use echocardiography (echo) or transesophageal (tranz-ih-sof-uh-JEE-ul) echo (TEE) as well as angiography (an-jee-OG-ra-fee) to guide them in threading the catheter to the heart and closing the defect. TEE is a special type of echo that takes pictures of the heart through the esophagus (the passage leading from the mouth to the stomach).
Catheter procedures are much easier on patients than surgery because they involve only a needle puncture in the skin where the catheter is inserted. This means that recovery is faster and easier.
The outlook for children having this procedure is excellent. Closures are successful in more than 9 out of 10 patients, with no significant leakage. Rarely, a defect is too large for catheter closure and surgery is needed.
Surgery
Open-heart surgery generally is done to repair primum or sinus venosus ASD. Your child is given medicine so that he or she will sleep through the surgery and not feel any pain.
During the surgery, the cardiac surgeon makes an incision (cut) in the chest to reach the ASD. He or she then repairs the defect with a special patch that covers the hole. Your child is placed on a heart-lung bypass machine so that the heart can be opened to do the surgery.
The outlook for children after ASD surgery is excellent. On an average, children spend 3 to 4 days in the hospital before going home. Complications, such as bleeding and infection, from ASD surgery are very rare.
Some children may develop inflammation of the outer lining of the heart, a condition called pericarditis (PER-i-kar-DI-tis). This causes fluid to collect around the heart in the weeks after surgery. This complication of a heart surgery usually resolves with medicine.
While in the hospital, your child will be given medicines as needed to reduce pain or anxiety. The doctors and nurses at the hospital will teach you how to care for your child at home.
They will talk about preventing blows to the chest as the incision heals, limiting activity while your child recovers, bathing, scheduling a follow-up medical appointments, and determining when your child can go back to his or her regular activities.
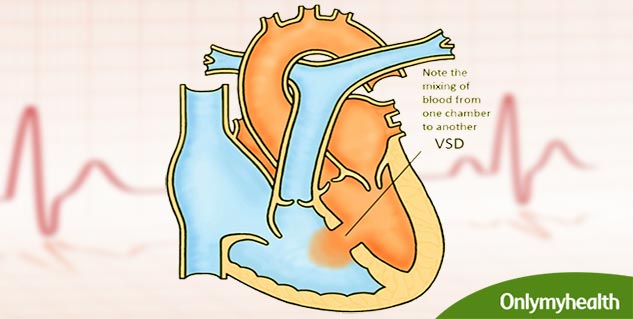
Treating Ventricular Septal Defect
Doctors may choose to monitor and observe children who have ventricular septal defects (VSDs) but don't have symptoms of heart failure. This means regular checkups and tests to see whether the defect closes on its own or gets smaller.
More than half of VSDs eventually close, usually by the time a child is in preschool. Your child's doctor will let you know how often your child should be checked. Checkups may range from once a month to once every 1 or 2 years.
When treatment for a VSD is required, options include extra nutrition and surgery to close the VSD.
The doctor may recommend surgery if your child's VSD:
- Is large.
- Is causing symptoms.
- Is medium-sized and is causing enlarged heart chambers.
- Affects the aortic valve.
Extra Nutrition
Some infants who have VSDs don't grow and develop or gain weight as they should. These infants usually:
- Have large VSDs.
- Are born prematurely.
- Tire easily during feeding.
Doctors usually recommend extra nutrition or special feedings for these infants. These feedings are high-calorie formulas or breast milk supplements that give babies extra nourishment.
In some cases, tube feeding is needed. Food is given through a small tube that's placed through the nose and into the stomach. Tube feeding can add to or take the place of bottle feeding. This treatment usually is temporary because a VSD that causes symptoms will likely need surgery.
Surgery
Most doctors recommend surgery to close large VSDs that are causing symptoms or haven't closed by the time children are 1 year old. Surgery may be needed earlier if:
- The child fails to gain weight.
- Medicines are needed to control the symptoms of heart failure.
Rarely, medium-sized VSDs that are causing enlarged heart chambers are treated with surgery after infancy. However, most VSDs that need surgery are repaired in the first year of life.
Read more articles on Heart Health.
For more related articles, download OnlymyHealth app.
How we keep this article up to date:
We work with experts and keep a close eye on the latest in health and wellness. Whenever there is a new research or helpful information, we update our articles with accurate and useful advice.
Current Version